Atrial fibrillation (AFib) is the most common irregular heart rhythm disorder. If the atria of the heart beats rapidly and irregularly, blood does not flow through the heart as quickly, according to the Cleveland Clinic. The irregular heartbeat makes the blood more likely to clot, and if the clot leaves the heart, it can travel to the brain and cause a stroke or to the coronary arteries and cause a heart attack.
There are several ways to treat AFib, including various medications, procedures such as electrical cardioversion and pulmonary vein ablation, and devices like pacemakers and left atrial appendage occluders.
Ablation procedures introduce a catheter into the left side of the heart and create circles of scar tissue around the pulmonary veins to isolate the veins from the rest of the atrium. The most common catheter-based technology in treating AFib is radiofrequency (RF) ablation, Jerry Melsky, VP of engineering at CardioFocus, told Medical Design & Outsourcing. In RF procedures, the physician typically repositions the catheter each time to make a lesion. The doctor may need to circle the pulmonary vein to make 50 to 100 lesions.
An alternative method is endoscopic laser ablation. In balloon technologies, the balloon goes in the vein, and once it’s stable, the physician can manipulate its energy source to make circles of lesions in as little as three minutes.
How to make an ablation catheter
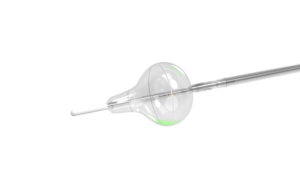
There are five elements in an endoscopic laser ablation catheter, such as CardioFocus’s HeartLight X3 system, allowing it to quickly ablate the pulmonary veins: the balloon, endoscope, sheath, laser energy source and motorized system.
The balloon is a compliant balloon that has an adjustable diameter. The physician places it right at the pulmonary vein entrance in the left atrium, feeding it through the body on the end of a catheter using a deflectable sheath.
A sheath guides the catheter and its device to the desired location. The HeartLight X3 ablation catheter, in fact, uses a sheath to deliver the balloon to the heart.
Endoscopes give physicians a real-time view of balloon deployment to ensure accuracy. They insert the fiber optic device into a catheter at the beginning of the procedure and remove it at the end. It is a small compact device that gives doctors a good visualization inside the vein, Melsky told MDO.
The laser energy in an ablation catheter like the HeartLight X3 makes permanent and durable lesions on the pulmonary vein to treat AFib. It’s possible to change laser energy dosing depending on where it is delivered to ensure that the vein is not over-treated or under-treated in any location.
A motorized system enables laser energy delivery in an automated fashion to make a continuous ring of lesions around the pulmonary vein “very quickly” in less than three minutes, according to Melsky.
The full ablation procedure starts with an ablation catheter inserted in the femoral vein and fed through a deflectable sheath that runs up the complete length of the inferior cava. The balloon threads through the inferior vena cava to the right atrium, where electrophysiologists do a transseptal procedure. They make a small puncture in the membrane that separates the left atrium from the right atrium. The catheter goes into the left atrium through the small puncture, with the balloon then deployed. Laser energy then ablates the afflicted pulmonary veins on the left side of the heart, creating circles of scar tissue to electrically isolate the pulmonary veins from the rest of the atrium.
Melsky said that the laser ablation technique is less time-consuming than other methods of ablation like RF.
“That takes a procedure that requires hundreds and hundreds of difficult maneuvers to make many lesions and turns it into a procedure where you only have to make a small number of maneuvers,” Melsky told MDO. “That small number of maneuvers is getting the balloon into each of the pulmonary veins.”
Overcoming technological challenges in making ablation catheters
It is important to understand the anatomy of the vasculature system, according to Melsky.
“We started out a while back trying to come up with a system that would make it very easy for the user to create lesions around the pulmonary vein, but there were a lot of unknowns at the beginning of the project,” Melsky said. “Probably the biggest unknown is, ‘What does the anatomy of the vein look like, and what does the interface between the balloon and the vein look like?’”
When prototyping the HeartLight X3 catheter, engineers started with a catheter system that didn’t have endoscopic visualization. As a result, the device didn’t work as well as the CardioFocus engineers had hoped. Without the imaging capabilities of the endoscope, they couldn’t see how the balloon was contacting the tissue around the pulmonary vein and where it delivered the laser energy.
Once the CardioFocus engineers incorporated the fiber-optic endoscope, they could see how the catheter system was working.
“We started to make progress really rapidly,” Melsky said. “You start to think that really doing this complicated ablation procedure in the pulmonary veins is so much easier and so much better and faster if you can get direct visualization of what you’re doing.”
The evolving catheter delivery device market
The evolution of catheter devices is ongoing, Melsky said. Balloon angioplasties, which involves a specialized catheter that delivers a stent to blocked arteries, kick-started the transformation, and the space continues to innovate.
“It’s more evolutionary than revolutionary,” Melsky said. “Whenever you have a specific problem that you have to solve, or if your focus is making atrial fibrillation safe, fast and effective, it will have a lot of value for the patient.”

