To achieve stiffness in intervascular catheter shafts, manufacturers often turn to stainless or nitinol – but those materials aren’t suited for MRI. Luckily, low-cost fibers offer a viable alternative.
William Li and Steve Maxson, Adam Spence

Intervascular catheter shafts are designed to be relatively stiff at the proximal end, to facilitate the pushing and torquing of the catheter as it advances through the body. The proximal shaft is joined with a flexible distal end to allow passage of the catheter tip through increasingly smaller vessels.
Typically reinforced catheter shafts are constructed using a composite design consisting of a lubricious inner liner material, such as PTFE or HDPE, for guidewire tracking; and an outer sheath, usually of Pebax, polyurethane or PA12 with varying durometers, from the proximal end to the distal tip. Non-reinforced catheter shafts are generally flimsy and require a continuous braid embedded in the catheter tubing to provide torquability and pushability while retaining flexibility and kink resistance. Most commonly, the braid is a metal such as stainless steel or nitinol.
Imaging issues
X-ray, including fluoroscopy and computed tomography (CT), are the common imaging methods in interventional cardiology. But fluoroscopy exposes the patient and medical personnel to ionizing radiation. This is an issue for the patient during repeat interventions (especially for children), and also for medical personnel, who must monitor their own dosage levels. In addition, fluoroscopy only generates a 2D projection.
Magnetic resonance imaging (MRI) presents several advantages over fluoroscopy in guiding cardiac interventions. MRI, which involves a complex interaction of magnetic and radiofrequency (RF) fields, does not use hazardous ionizing radiation, allowing for repeated scans. And MRI scans can be oriented in three dimensions in real time, providing high-resolution soft-tissue contrast compared to X-ray-based imaging.
The traditionally metallic braiding materials embedded in catheter shafts are ferro-magnetic and therefore not compatible or safe to use with MRI. These ferro-magnetic metals cause signal loss (artifacts) and result in MRI image distortion. Beyond these visibility issues, there are safety risks from the force exerted by the magnetic field on the metal in the braiding and RF-induced heating of the metallic braid reinforcement incorporated into the catheter.
In one study performed by Losey AD et al. in 2014 at UCSF’s Dept. of Radiology & Biomedical Imaging, different braid materials were analyzed during MRI scans at 1.5 Tesla and 3 Tesla. During a 15-minute scan, nitinol braid showed a temperature increase of 0.45°C at 1.5 Tesla and 3.06°C at 3 Tesla; subsequent tests for tungsten- and PEEK-braided catheters showed no heating during scans.
Braiding requirements
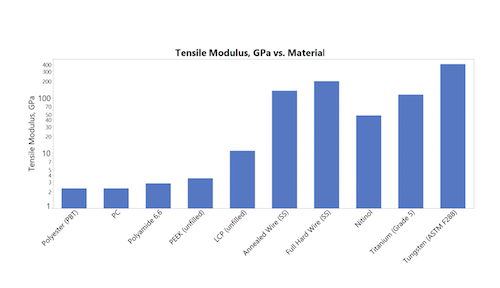
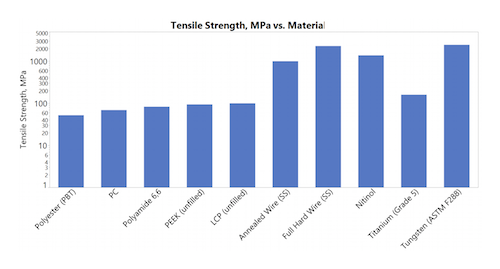
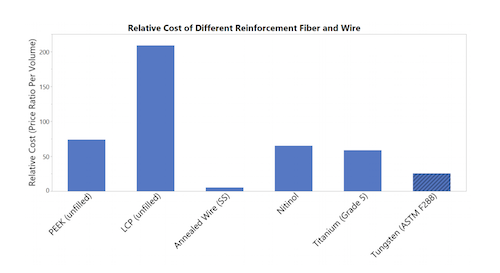
Braid material requirements include biocompatibility, radiopacity, tensile strength, tensile modulus and material cost. Charts with this article show the mechanical properties (tensile modulus and tensile strength), as well as the relative costs of monofilament and braid materials.
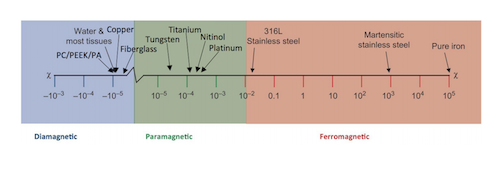
Another important property for MRI compatibility is the braid material’s magnetic susceptibility, or the measure of the propensity of the material to become magnetized when placed in the magnetic field. This article’s final chart shows the magnetic susceptibility of common fibers and metallic braid materials. Polymers and human tissue are MRI-compatible with very low magnetic susceptibility indices (<1×10-5, diamagnetic) and very little image distortion even if they are very close to the imaging region. MRI-incompatible stainless steel has a high magnetic susceptibility index (>1×10-2, ferromagnetic), meaning image distortion even when it is very far from the imaging region.
Because different modalities may be used to navigate the vasculature, it’s desirable to have a catheter shaft that is both radiopaque for fluoroscopy and has low magnetic susceptibility for MRI.
Performance fibers
Titanium and tungsten are biocompatible and X-ray- and MRI-compatible. They have relatively low magnetic susceptibility indices and only distort images if they are very close to the imaging region. Tungsten is a high-density metal (70% more dense than lead) and therefore highly radiopaque. It also boasts high tensile modulus and strength and is less expensive than other precious metals such as titanium or platinum.
Most polymer-based braid materials do not include radiopaque fillers, because the loading levels of radiopaque filler required for visibility (~20%) would likely adversely affect fiber strength. Current development studies include hybrid structures combining the superior mechanical properties of metals with MRI-compatible polymers.
Beyond the mechanical performance of tungsten wire, a catheter shaft reinforced using tungsten offers the versatility of whole-shaft X-ray and MRI visibility from the proximal end to the radiopaque distal tip at a lower price compared with high-performance polymer materials such as PEEK or LCP.
Lower-cost fiber such as PET, Nylon or PC can be used when the dimensions (diameter and wall thickness) of the catheter allow the fiber to have a relatively large cross section. For example, one design could include a metallic marker band and a few strands of tungsten wire to enhance radiopacity and MRI visibility.
Influence on manufacturing process
Monofilament fiber and metallic wire can be braided using a Steeger-type braider at speeds of up to 400 rpm. When there is a size limitation on the wall thickness of a catheter, the filament/wire size needs to be smaller. Small fiber such as 0.002-in. monofilament may need to be braided at lower speeds (175rpm to 225rpm) to avoid constant breaking and fraying.
Conclusion
MRI offers substantial benefits for radiation-free noninvasive visualization of reinforced catheter shafts in the vascular system. Braid materials in the form of high performance polymers and non-magnetic metals imbedded within the catheter provides the optimization of physical properties and minimized localized heating and image artifacts under MRI. Non-magnetic metallic braid materials that are both X-ray- and MRI-compatible are very good options due to their lower costs and easier processability compared to most high-performance polymer braid materials. Metallic materials can be braided at high speeds compared to some polymer braid materials, potentially resulting in higher throughput and overall lower braiding machine capital equipment costs.
William Li is an R&D engineer at Adam Spence (formerly Fermetex Vascular Technologies) in Wall, N.J. Li works closely with sales and marketing in new business development. He has worked in the medical device industry for 22 years, 18 years of which was with W.L. Gore & Associates focusing on catheter technology and product development.
Steve Maxson is VP of marketing and sales at Adam Spence (formerly Fermetex Vascular Technologies) in Wall, N.J. Prior to joining Adam Spence, Steve served in various leadership roles at American Kuhne for over 15 years, most recently as director of global business development.
The opinions expressed in this blog post are the author’s only and do not necessarily reflect those of MedicalDesignandOutsourcing.com or its employees.
